General Physiotherapy
What is Physiotherapy?
What does it involve?
- Advice – Diagnosing the problem through a thorough clinical examination and letting you know what to expect and how to manage yourself through the recovery
- Mobilisation – Hands on treatment to mobilise stiff and painful joints from grades I-IV.
- Manipulation – A grade V mobilisation technique to achieve full range of movement of a joint, similar to that used by Chiropractors and Osteopaths, only possible after grade IV mobilisation has been achieved. Otherwise known as a High Velocity Thrust.
- Acupuncture – involves inserting thin, sterile needles into specific acupuncture points on the body to decrease tissue inflammation, reduce pain and promote healing. More about acupuncture.
- Trigger Point Needling – A method used to treat pain and dysfunction caused by muscle and nerve problems using very thin, solid needles, with no medication (i.e. a dry needle) as used in acupuncture, which is based on western medical principles and scientific research.More about trigger point needling.
- Pilates – Body conditioning system of exercise which stabilises the body’s central core and improves posture. At spinalphysio Pilates is carried out on a one to one basis with a suitably qualified chartered physiotherapist.
- Exercise – A physiotherapist can design an exercise programme to suit your personal needs and limitations. Exercise can be very important at keeping you right but it may not get you right. It is very important that a physiotherapist assess and if necessary treats your particular injury before recommending a suitable exercise program.
- Postural Education – Helping people to become aware of their posture and improve their posture, by finding ways to remember to regularly check and improve their position, and through exercises to strengthen certain muscle groups
- Ergonomics – Determining what equipment is needed, and in what way it should be used, to avoid muscular strain and repetitive strain injuries, taking into account people’s capabilities and limitations
- Strapping – applying taping techniques to protect injured parts, control or limit movement.
If you would like to book an appointment please email info@spinalphysio.co.uk or call 01223 350622
Our General Physiotherapy Services

Neck Pain
Show More
As a result of increased dependence on computers, more time is being spent at a computer each working day. It is very important that the work station is set up correctly to allow the minimum of stress through the joints. An occupational health adviser can help address any concerns you may have with the help of the physiotherapist if necessary.
Looking after your posture can go along way to helping ease the discomfort. Making sure you move away from static postures regularly helps. Stand up and have a stretch every 20 minutes at work or when watching television at home. Make sure your looking directly straight on at the computer or television and that the screen is at the correct height. Don’t hold the mouse or gear lever in your hand when your not using it and don’t put your elbow up on the window of the car when driving.
Postural neck ache can usually easily be treated with some gentle mobilisation by a physiotherapist and a stretching program to prevent recurrence. You can also prevent its onset by following the same advice as given for low back ache
Sit up properly and arrange your work station to best suit your height and shape.
Stand up every 15-20 minutes to recover the arch in your spine, both at home and at work.
Go for a long walk (40 minutes) per day, ideally in one go or split it in two, 20 minutes at lunch and 20 minutes when you finish work.
Try to stretch regularly through the day.
Don’t drive for greater than one hour without getting out to stretch your legs.
See a Chartered Physiotherapist if you have pain that doesn’t settle down in 48 hours.

Trapped Nerve
Show More
Your doctor may also prescribe anti-depressants at a low dose as these can sometimes help with nerve pain and also help people sleep and it is not necessarily because you are depressed. Physiotherapy can be useful in mobilising the spine safely to un-trap the nerve and should be considered if there is no improvement in pain in the first 48 hours.

Myofascial Pain
A trigger point is active when it is causing pain and twitches when compressed. A common area of the body susceptible to trigger points are the muscles connecting the shoulders to the neck or upper trapezius muscles.
Show More
To treat the trigger point the physiotherapist has a couple of options. They may try some myofascial release which will involve deep tissue palpation of the trigger point in order to desensitise it. Another option is to treat the area with what is known as trigger point needling. This involves putting a fine needle (usually an acupuncture needle although it is not acupuncture) into the muscle to deactivate the trigger point. An acute spasm is felt in the muscle and a release of tension follows. You will then be shown how to stretch the muscle and this will have to be carried out regularly. Trigger point needling may be very effective in one session or may take a number of sessions to fully resolve the pain depending on the severity of the problem.
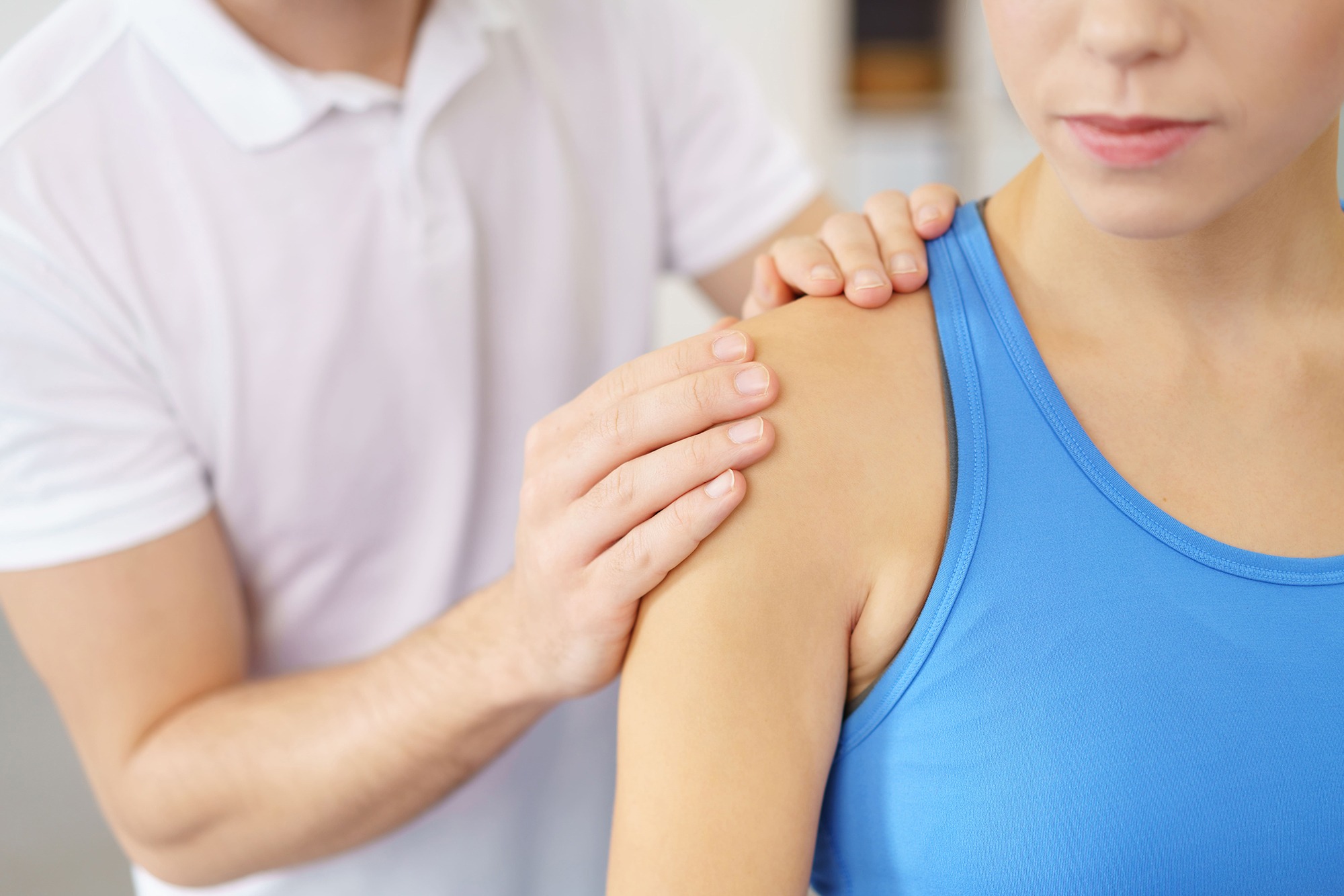
Shoulder Impingement
Any one or more of a number of structures can get pinched in this space. Usually one of two structures are involved. Most frequently it is a tendon of the rotator cuff. The rotator cuff is a group of four muscles coming from the spine and shoulder blade. They wrap around the shoulder joint to suck the ball of the shoulder into the socket of the joint. They give stability to the joint and are also involved in the movements of the arm particularly rotation as the name would suggest.
Show More
The tendon that is most exposed in the rotator cuff is the supraspinatus tendon. This tendon lifts the arm away from the body and helps rotate it away from the body. When the arm is lifted overhead the tendon can become squeezed between the shoulder joint and the Acromioclavicular joint on the top of the shoulder. If this happens once or twice it is not a great problem. Repeated catching of this tendon will cause it to become inflamed. That results in a tendonitis making the shoulder painful, weak and increasingly stiff.
If the tendonitis is not treated early it can cause a chronic impingement of the shoulder. Prolonged inflammation will weaken the tendon and could eventually cause the tendon to fray or tear. The tendon can also be torn as a result of trauma such as a fall on an outstretched hand or onto the shoulder. If the arm is suddenly forced backwards or rotated this could also tear the tendon or by lifting something too heavy or repetitive overhead lifting. A torn rotator cuff tendon is a painful and debilitating injury that can take months to years to resolve.
It is important to ask why the tendon would become squeezed between the shoulder and AC joints in the first place. Normally there is enough space between these joints for the arm and tendons to function properly. So what would cause the space to narrow? The most common reason is posture. If you allow your shoulders to slouch forward as when sitting at a PC or folding your arms in front of your chest, this will narrow the joint space. This is a gradual process and slowly causes the shoulders to become rounded and will eventually cause an impingement. Another possibility is degenerative wear and tear of the AC joint. If the AC joint becomes worn, small boney projections called osteophytes can protrude from the joint. These act like little daggers into the soft tissues under the joint. Both of the scenarios above will result in a shoulder impingement.
The other structure in the Acromioclavicular joint space that gets squeezed is the sub acromial bursa. This is a fluid filled sack much like an airbag that sits between the rotator cuff and the point of the shoulder. It is there to act like a shock absorber in the joint. If there is repetitive squeezing of the bursa it can slowly become inflamed. It will also become acutely inflamed as a result of direct trauma such as a fall onto the arm compressing the joint or if something falls onto the shoulder from above.
The swollen bursa will reduce the space between the shoulder joint and the Acromioclavicular joint and will be squeezed or pinched when the arm is raised. This also causes an impingement syndrome.
Depending on the source of the impingement there are different ways to treat the problem. Firstly it is important to establish the correct diagnosis. The physiotherapist has a number of clinical tests they can carryout to help achieve this. If they are unsure or need to confirm the diagnosis it may be necessary to carry out other tests. An x-ray of the shoulder can identify or rule out the possibility of an osteophyte. An MRI scan may be able to establish a tear in the rotator cuff or a swollen bursa. Ultrasound scans are also useful to see the rotator cuff in various positions as it is possible to move the shoulder while carrying out an ultrasound scan. This is not possible when performing an MRI scan. One or more of these tests may be required to finalise a diagnosis.
Once the correct diagnosis is established the treatment begins. An acute tendonitis can be treated with Ice, anti-inflammatories and an exercise program. A traumatic rotator cuff tear needs to be placed in a sling and rested for about 3 weeks. Also during this time the physiotherapist will work on the tendon to prevent the formation of scar tissue and then rehabilitate the shoulder girdle complex when appropriate.
A bursitis may need a cortisone injection to kill the inflammation but the physiotherapist can normally reduce the pressure on the bursa by mobilizing the joint and strengthening the shoulder. Impingements as a result of posture or osteophyte formation need a lot of work on improving posture and mobilising the Acromioclavicular joint to improve joint space. The underlying tendonitis or bursitis also needs to be treated and the shoulder rehabilitated.
If conservative management is not effective then other interventions such as injection therapy or surgery are available. Most surgeons will tell there patients to try conservative management for at least 3 months before resorting to surgery and will often insist on waiting a year before operating.

Frozen Shoulder
There are two types of frozen shoulder. Primary or idiopathic frozen shoulder is of unknown cause. It classically occurs in females more than males and in those usually over 45 years of age. It will normally be in the non dominant arm and is more likely to occur in those in a sedentary profession. Secondary frozen shoulder follows significant trauma to the shoulder such as a fracture, dislocation or severe burn. However this injury may have occurred some years previously.
Show More
A frozen shoulder will run 3 stages. Stage 1 is the freezing phase where the shoulder becomes increasingly stiff and painful. Phase 2 is the frozen phase where the shoulder is so stiff that it will not move above shoulder height. This is often the most painful stage and it is then people will usually seek help for the shoulder. It is painful to sleep on and the shoulder usually becomes very sensitive even to small changes in movement. The third and final stage is the thawing phase when the pain reduces and the movement slowly improves.
Each stage of a frozen shoulder will last from 4 to 8 months. Therefore taking anywhere from 1 to 2 years to resolve. Frozen shoulders will solve themselves eventually and will never occur again in the same shoulder. There is unfortunately a 13% chance of it occurring on the other arm, usually within a year of the initial shoulder resolving.
Treatment for a frozen shoulder will vary depending on what stage you are at. In the early phase it is important to try to maintain the movement and control the pain. Anti-inflammatory medication may be useful or even a cortisone injection. There is some debate as to the presence of inflammation in frozen shoulder but research is split on the topic. Physiotherapists can help to control pain and maintain movement.
In the second and most painful stage aggressive manual therapy is counter productive. Patients try a variety of modalities to help ease the pain such as ice or heat or electrotherapy. There is evidence for and against each of these. Whatever works best for the individual should be continued. The aim of treatment at this phase is to control the pain. Acupuncture has been shown to be the most effective. Your physiotherapist may be able to perform this for you or refer you to a suitably qualified person.
In the third phase the pain drifts away and it is then time to get the joint moving. Mobilisation of the joint should be carried out by the Physiotherapist and an exercise program established to get you back to full function.
There are surgical options for frozen shoulder but these are carried out rarely and like everything else in frozen shoulder are debatable. Manipulation under anesthetic is carried out to try to break any adhesions in the joint and kick start the movement. Other more invasive procedures attempt to release the capsule covering the joint in order to free some movement.

Carpal Tunnel Syndrome
The median nerve is one of many nerves in the arm. It supplies power to some of the muscles in the hand and also sensation to the thumb, index finger, middle finger and half the length of the ring finger on each hand.
Show More
Most people with carpal tunnel syndrome complain of pins and needles in the hand and fingers especially in the morning and this may even wake them at night. The hand or hands often feel heavy and numb and they will have to shake them out to “get them going in the morning”. The symptoms may also be aggravated throughout the day if there is a build up of pressure in the wrists for any of the reasons mentioned above.
In order to treat carpal tunnel syndrome the main cause needs to be established. In an office environment incorrect keyboard or mouse use can be a very significant factor. Adjusting the hand, wrist and forearm position so that the hand is in a relaxed and neutral position allows all the structures to pass through the carpal tunnel with the greatest of easy. If you are unsure of how to achieve this contact a Chartered physiotherapist who can arrange a work station assessment for you.
If sleeping is the biggest problem wrist splints can be useful which help keep the wrist in a neutral position overnight so that the median nerve does not get squeezed during the night if you bend your wrist while you sleep. However, if localised swelling is the source of the problem, such swelling is often worse at night and splints may be of limited use. If swelling is a factor then the source of that swelling needs to be address either with appropriate medication as prescribed by your GP or a steroid injection by a specialist.
Physiotherapy can help to identify the correct diagnosis and cause of the problem and may also be able to treat the source of the problem. If all else fails there is a simple surgical procedure which can release the pressure in the tunnel and “fix” the problem.
Remember that carpal tunnel syndrome is not the only cause of pins and needles in the fingers and a thorough assessment is necessary to establish the correct diagnosis.
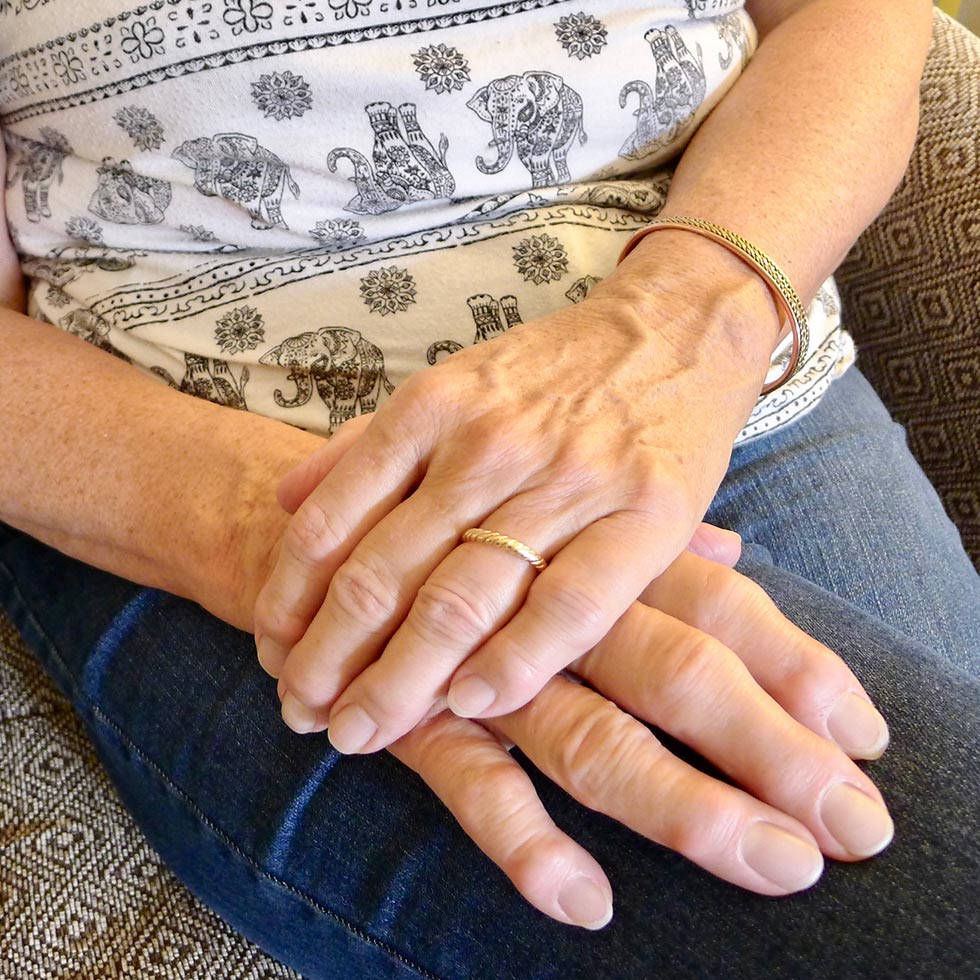
Arthritis Of The Wrist & Hand
Relatively minor stress to the bone is often classified as wear and tear. If this stress is as a result of trauma, such as a fall where there is bone pain but no fracture, it may be a bone bruise. Stress from repeated weight bearing on the joints may cause wearing of the cartilage covering the bones, leading to wear and tear / osteoarthritis, which can progress into inflammatory arthritis.
Show More
The tendon that is most exposed in the rotator cuff is the supraspinatus tendon. This tendon lifts the arm away from the body and helps rotate it away from the body. When the arm is lifted overhead the tendon can become squeezed between the shoulder joint and the Acromioclavicular joint on the top of the shoulder. If this happens once or twice it is not a great problem. Repeated catching of this tendon will cause it to become inflamed. That results in a tendonitis making the shoulder painful, weak and increasingly stiff.
If the tendonitis is not treated early it can cause a chronic impingement of the shoulder. Prolonged inflammation will weaken the tendon and could eventually cause the tendon to fray or tear. The tendon can also be torn as a result of trauma such as a fall on an outstretched hand or onto the shoulder. If the arm is suddenly forced backwards or rotated this could also tear the tendon or by lifting something too heavy or repetitive overhead lifting. A torn rotator cuff tendon is a painful and debilitating injury that can take months to years to resolve.
It is important to ask why the tendon would become squeezed between the shoulder and AC joints in the first place. Normally there is enough space between these joints for the arm and tendons to function properly. So what would cause the space to narrow? The most common reason is posture. If you allow your shoulders to slouch forward as when sitting at a PC or folding your arms in front of your chest, this will narrow the joint space. This is a gradual process and slowly causes the shoulders to become rounded and will eventually cause an impingement. Another possibility is degenerative wear and tear of the AC joint. If the AC joint becomes worn, small boney projections called osteophytes can protrude from the joint. These act like little daggers into the soft tissues under the joint. Both of the scenarios above will result in a shoulder impingement.
The other structure in the Acromioclavicular joint space that gets squeezed is the sub acromial bursa. This is a fluid filled sack much like an airbag that sits between the rotator cuff and the point of the shoulder. It is there to act like a shock absorber in the joint. If there is repetitive squeezing of the bursa it can slowly become inflamed. It will also become acutely inflamed as a result of direct trauma such as a fall onto the arm compressing the joint or if something falls onto the shoulder from above.
The swollen bursa will reduce the space between the shoulder joint and the Acromioclavicular joint and will be squeezed or pinched when the arm is raised. This also causes an impingement syndrome.
Depending on the source of the impingement there are different ways to treat the problem. Firstly it is important to establish the correct diagnosis. The physiotherapist has a number of clinical tests they can carryout to help achieve this. If they are unsure or need to confirm the diagnosis it may be necessary to carry out other tests. An x-ray of the shoulder can identify or rule out the possibility of an osteophyte. An MRI scan may be able to establish a tear in the rotator cuff or a swollen bursa. Ultrasound scans are also useful to see the rotator cuff in various positions as it is possible to move the shoulder while carrying out an ultrasound scan. This is not possible when performing an MRI scan. One or more of these tests may be required to finalise a diagnosis.
Once the correct diagnosis is established the treatment begins. An acute tendonitis can be treated with Ice, anti-inflammatories and an exercise program. A traumatic rotator cuff tear needs to be placed in a sling and rested for about 3 weeks. Also during this time the physiotherapist will work on the tendon to prevent the formation of scar tissue and then rehabilitate the shoulder girdle complex when appropriate.
A bursitis may need a cortisone injection to kill the inflammation but the physiotherapist can normally reduce the pressure on the bursa by mobilizing the joint and strengthening the shoulder. Impingements as a result of posture or osteophyte formation need a lot of work on improving posture and mobilising the Acromioclavicular joint to improve joint space. The underlying tendonitis or bursitis also needs to be treated and the shoulder rehabilitated.
If conservative management is not effective then other interventions such as injection therapy or surgery are available. Most surgeons will tell there patients to try conservative management for at least 3 months before resorting to surgery and will often insist on waiting a year before operating.

Posture
Posture can be classified into 5 main categories. Unfortunately it’s not that simple.
Each category can be further classified into a number of sub groups which go to form your posture type. Everybody falls into a main category and then a combination of sub groups. So although you may have been told you are a certain posture type and been advised to do exercises for that type, they may not be correct for your sub group. A chartered physiotherapist is the expert in assessing your posture and advising accordingly.
Perfect posture is a difficult goal to achieve but the closer you are to perfect the better your body will feel and perform.
Online Consultation
We understand it’s not always possible to get to the clinic or you just have some questions that you’d like to discuss with an expert and get some advice.
With an online consultation you can have a 30 minute Zoom/Skype appointment with an experienced Chartered Physiotherapist who will discuss your concerns and offer appropriate advice.
